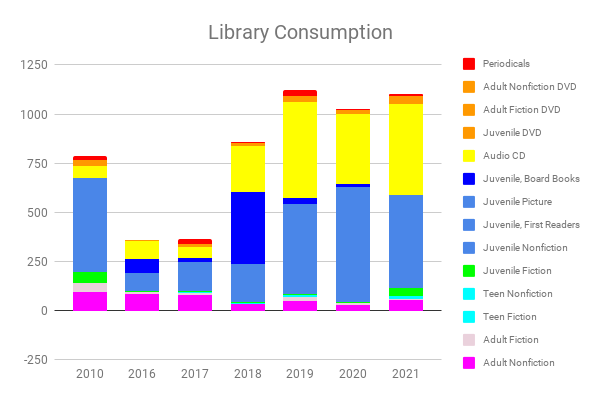
We officially called wraps on the 2021-2022 school year in the middle of June – we’ll be back at it next week, Lord willing. But even once we were officially “done”, we continued morning time – it’s something of an anchor for our days.
For us, morning time has been a matter of “if it ain’t broke, don’t fix it.” I started doing morning time as soon as I finished breakfast but while the kids were still dawdling over it sometime in the 2019-2020 school year and it has continued to work well for us.
Morning Worship
We start morning time with the Scriptures. I open with “Let’s hear what God’s Word says” and then read a passage, closing with “This is the Word of the LORD”, to which we all reply “Thanks be to God.” This is our church’s customary formula for Scripture readings and we want our children to be comfortable with the format.
I added Scripture memory to our rotation in January – I had been intending to do so but had a hard time arriving at a perfect system. Finally, I decided that, despite not having a perfect system we were going to just jump in. We practice the children’s current memory verses from Sunday school daily and then practice 2 “back verses” from the preschool repertoire at church and 2 back verses from the ones that go along with Tirzah Mae and Louis’s Sunday school class.
Also in January, we started working on the New City Catechism as a family during our evening worship, so I review a couple of back questions and answers and we listen to and sing along with the song for the current question.
Daniel and I have long agreed that we think memorizing extended passages of Scripture is ideal for retention, understanding, and application, so for our last interval, I added a longer Scripture passage for us to memorize. We practiced Psalm 1 right after our Scripture reading – and there’s little more delightful than hearing Shiloh leading the others in “are like chaff, which the wind drives away.” This seemed to work well and I hope to memorize one short passage per interval in our next school year.
This year, we read the Psalms and Proverbs, memorized Psalm 1, and memorized the first 22 questions of the New City Catechism.
Poetry and Nonsense
Our next section is on the silly side. We start with a nursery rhyme, then read a poem, then a few jokes, and end with some trivia.
We’ve read all of the nursery rhyme collections our library owns, so I’m just cycling through the three I own and enjoy: Kate Greenaway Nursery Rhyme Classics, Tomie DePaola’s Mother Goose,, and The Glorious Mother Goose. We got through all three this year.
For our poetry, I check out a book of poems from the library (Dewey Decimal system 811, Children’s Nonfiction). When we finish, I check out another. If I happen to not have another queued up when we finish one book, I grab a collection we own and read the next poem in that collection until we’ve got another library book to peruse.
Poetry Read:
- R is for Rhyme: A Poetry Alphabet by Judy Young
- Lots of Spots by Lois Ehlert
- You and Me: Poems of Friendship by Sally Mavor
- Dinosaur Dances by Jane Yolen
- Animal Fare by Jane Yolen
- Sleigh Bells and Snowflakes compiled by Linda Bronson
- The Stable Rat and other Christmas Poems by Julia Cunningham
- The Glorious Christmas Songbook by Cooper Edens and Benjamin Darling
- At Christmastime by Valerie Worth
- Bird Watch by Jane Yolen
- Water Music by Jane Yolen
- Dear Mother, Dear Daughter by Jane Yolen and Heidi Stemple
- Birds of a Feather by Jane Yolen
- A Child’s Garden of Verses by Robert Louis Stevenson
Reading jokes at morning time began when Daniel was traveling at the end of 2020 and would send the kids voice messages with knock knock jokes. The kids enjoyed them and I realized that puns are a pretty great learning opportunity too (hearing Louis giggle at a joke as he says “It should be ‘joke’ instead of ‘yolk'” is pretty great.) Just like with the poems, I check a book out of the library, we read it, and then I check another out. If I happen to plan poorly and run out of jokes, we just go without.
Joke Books Read:
- My First Knock-Knock Jokes by Jimmy Niro
- Bell Buzzers: A Book of Knock-Knock Jokes by Michael Dahl
- Nutty Neighbors: A Book of Knock-Knock by Michael Dahl
- Doctor, Doctor: A Book of Doctor Jokes by Michael Dahl
- Family Funnies: A Book of Family Jokes by Michael Dahl
- School Buzz: Classy and Funny Jokes about School by Michael Dahl
- Teacher Says: A Book of Teacher Jokes by Michael Dahl
- The Classroom Zone: Jokes, Riddles, Tongue Twisters & “Daffynitions” by Gary Chmielewski
- Let’s Eat in the Funny Zone: Jokes, Riddles, Tongue Twisters & “Daffynitions” by Gary Chmielewski
- The Medical Zone: Jokes, Riddles, Tongue Twisters & “Daffynitions” by Gary Chmielewski
- The Science Zone: Jokes, Riddles, Tongue Twisters & “Daffynitions” by Gary Chmielewski
- Ribbit Riddles by Katy Hall and Lisa Eisenberg
- ABC Animal Riddles by Susan Joyce
- Otter Nonsense by Norton Juster
Finally, we enjoy some trivia. I’m not sure when or how we started, but we began reading a “did you know” book at the end of morning time and discovered that we really enjoyed learning random little things. We’ve mostly been writing through the National Geographic Kids series “Little Kids First Big Book of…”
Trivia Read
- National Geographic Kids Little Kids First Big Book of Why 2 by Jill Esbaum
- National Geographic Kids Little Kids First Big Book of Why by Amy Shields
- National Geographic Kids Little Kids First Big Book of Science by Kathleen Weiner Zoehfeld
So What’s Next?
When we start up again, I plan to continue on as we have been with only a couple of adjustments. We’re going to add some extra memory work between our catechism review and nursery rhymes (we practiced my phone number and our address during our last interval and I think we’ll start with the books of the Bible for the next school year.) I also feel like morning time sometimes ends with a whimper when attention starts to wane on our trivia – I’d like to finish off more decisively with a hymn. Then there’s a clear “we’re done” to mark the transition from the table and to chores.