Each time we did a biophysical profile and the ultrasound tech let me know that baby was head down, I marveled a little internally that this time it didn’t matter.
Having a head-down baby really mattered when I was aiming for a VBAC (vaginal birth after cesarean) and a VBA2C (vaginal birth after two cesareans). But presentation means next to nothing when you’re planning a pre-labor cesarean due to complete placenta previa.
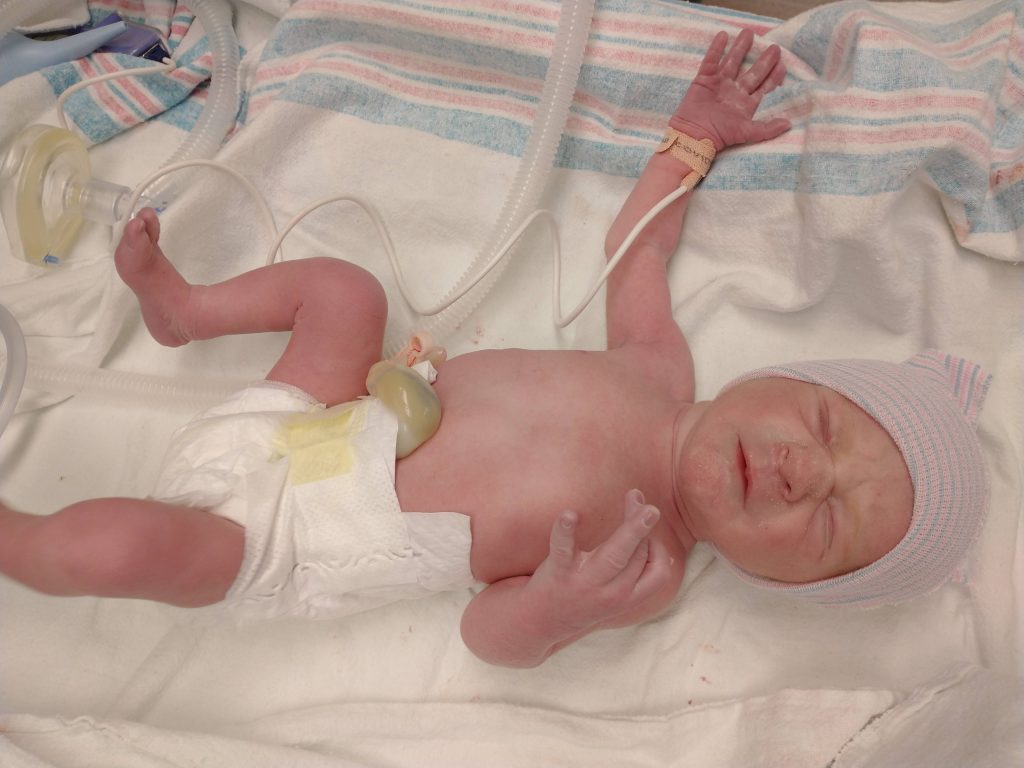
But then my blood pressure rose to severe ranges and I headed to the hospital.
Hospital staff were getting everything prepped for our c-section when they rolled in the ultrasound to take one last look at the placenta. It’d been three weeks since we’d looked at it directly – it hadn’t moved in the dozen weeks before that and we felt sure it wasn’t going to. What’s more, a regular ultrasound a couple weeks before had the ultrasound tech cautiously feeling out whether I knew the placenta was not going to let me VBAC this time. The previa was a done deal. It wasn’t moving. But it’d still be good to take a good look before we head to surgery.
But the tech couldn’t find the placenta on transvaginal ultrasound. It wasn’t over my cervix anymore. A regular abdominal ultrasound showed the placenta four centimeters behind my cervix. No previa.
And baby was head down, which suddenly mattered again. I no longer had an absolute contraindication for vaginal delivery! I was free to “TOLAC” again (trial of labor after cesarean).

So we started an induction. After an hour or two (maybe?), my blood pressure wasn’t coming down with IV labetalol so we decided to start an epidural sooner rather than later in hopes that it would bring my blood pressure down (I had already planned to get an epidural this time around since it would be an induced labor, which generally means more pain, and because I wanted the “insurance” of an epidural in place in case we needed to rapidly transition to a cesarean.) So we got the epidural in.
“Woo-ooo,” I let the anesthesiologist know that I was feeling woozy. The blood pressure cuff that had been inflating and deflating on my arm since admission confirmed that my blood pressure had dropped, quite low. The staff laid me down; they pushed fluids through my IV ports; they gave me medicine. I stabilized.
They rearranged the belly monitors, trying to get baby’s heart rate back on the monitor – but they couldn’t find it. Quick, bring in a ultrasound – oh, that explains it. Heart’s beating just fine, but baby is breech now. “What’s his presenting part?” I asked. “Foot” was the response.
A footling breech. Not even my doc, who does deliver breech babies vaginally under some circumstances, would deliver a footling breech vaginally.
For the second time that day, we began preparations for a c-section.
In the half hour it took my doctor to get from his west side office (of course this all had to happen when he wasn’t just across the street like he is at the beginning of the week!) back to the hospital to perform the c-section, Frank had flipped again, this time to transverse (lying across my belly rather than up and down).

And so Frank was born, via a plan D c-section for breech positioning. He broke a collarbone on the way out (gotta be careful with those gymnastics!) but it hasn’t seemed to have bothered him.
I can’t help thinking of the parallels and perpendicularities between Louis’s birth and Frank’s.
With both, I developed preeclampsia which subsequently developed severe features which necessitated delivery. With Louis, I was determined to do anything possible to avoid a repeat c-section – with Frank I had come to peace with the reality that vaginal delivery was completely out of the question. When our “last ditch” ultrasound showed Louis still transverse, we called in the specialist and did a version. Our “last ditch” ultrasound with Frank started us off on a surprise TOLAC. But Louis bobbed quickly head down and back up to transverse on his version and Frank flipped footling and transverse just because.
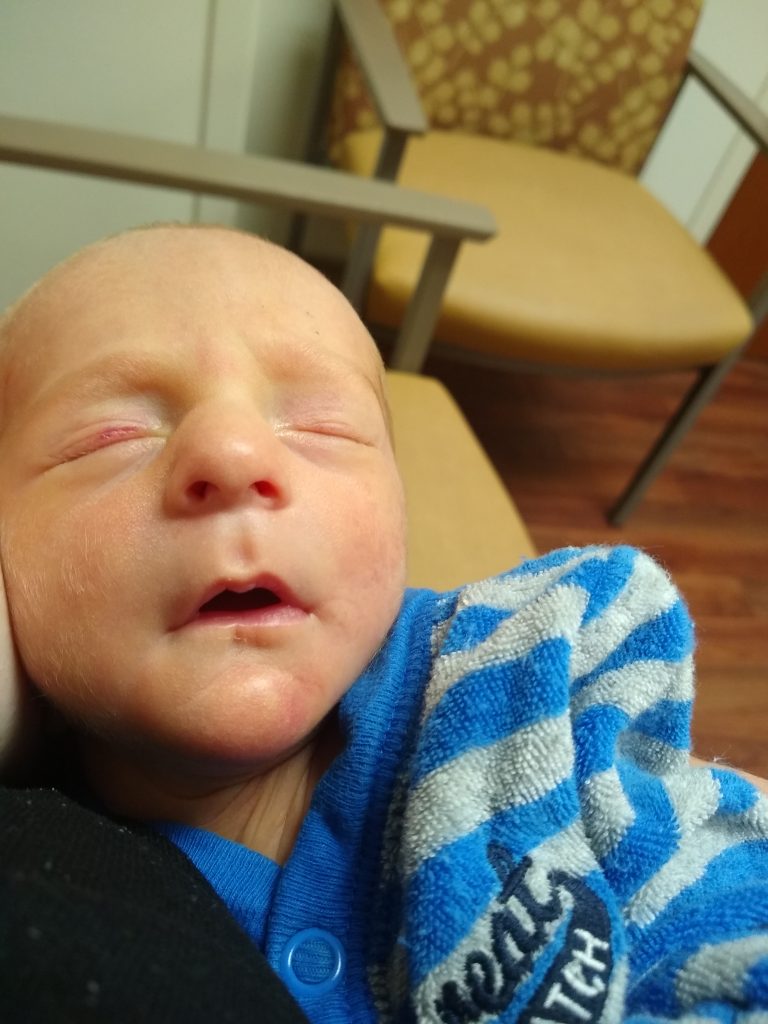
And both my breech boys were born via c-section, with stories specially written by a gracious God.



